![]() The Centers for Disease Control and Prevention (CDC) issued new guidance to people with weak immune systems, saying they should take extra precautions after a key COVID-19 antibody treatment’s emergency use authorization was pulled by another federal agency.
The Centers for Disease Control and Prevention (CDC) issued new guidance to people with weak immune systems, saying they should take extra precautions after a key COVID-19 antibody treatment’s emergency use authorization was pulled by another federal agency.
The guidance again calls for immunocompromised individuals to wear masks and engage in social distancing, the CDC’s revised guidance says, despite CDC-cited studies and data suggesting that masks provide little effectiveness in blocking the transmission of COVID-19. Some former federal officials have said that the six-foot social distancing rule adopted around the United States in early 2020 was arbitrary.
Last week, the U.S. Food and Drug Administration (FDA) pulled its authorization of Evusheld, a combination antibody treatment that is given to people with weak immune systems. The agency said that it is not effective against most of the COVID-19 Omicron subvariants that are currently circulating around the United States, including the XBB subvariants and the BQ strain.
“Among persons with immunocompromise and their household members and close contacts, prevention measures including wearing a high-quality and well-fitting mask, maintaining physical distance from others (at least six feet), improving indoor ventilation, practicing frequent handwashing, and developing a care plan, should be considered in addition to receipt of a bivalent booster dose,” said the CDC on Jan. 27.
The agency added that “it is important to wear a mask and maintain physical distance from others if it is not possible to avoid crowded indoor spaces … simple interventions should be used to improve ventilation in buildings and decrease SARS-CoV-2 transmission by improving air flow.” The agency also again recommended that immunocompromised people should get up-to-date COVID-19 vaccines.
The CDC advises that people who have a weak immune system and develop COVID-19-like symptoms to get tested for the virus. They should then receive an antiviral drug within five to seven days.
“Early outpatient treatment of mild to moderate COVID-19 with a recommended first-line therapy, ritonavir-boosted nirmatrelvir (Paxlovid), or remdesivir (Veklury), or the second-line therapy, molnupiravir (Lagevrio), have been shown to reduce the risk for severe COVID-19, including hospitalization and death,” it says. Some doctors have expressed concerns about remdesivir, claiming the drug has potentially fatal side-effects like kidney failure.
About 7 million people in the United States have a condition that greatly compromises their immune system, such as cancer, according to CDC figures.
FDA Pulls Authorization
Evusheld, which the FDA pulled on Jan. 26, is manufactured by AstraZeneca, and it was first authorized in December 2021 as a pre-exposure prophylaxis against COVID-19 for people with weak immune systems and aren’t likely to generate COVID-19 antibodies via vaccination.
The agency said that as of now, the drug cannot neutralize a number of Omicron subvariants like BQ.1, BQ.1.1, BF.7, BF.11, BA.5.2.6, BA.4.6, BA.2.75.2, XBB, and XBB.1.5.
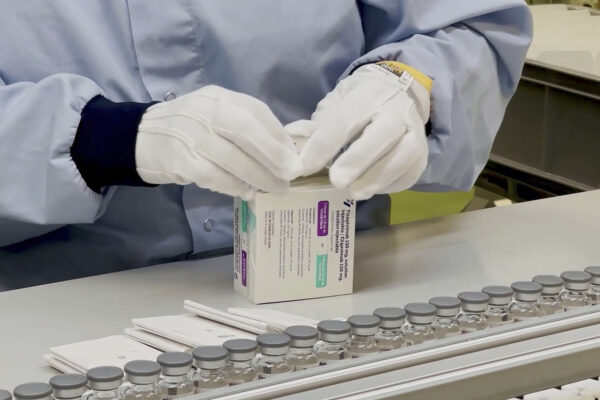
“This means that Evusheld is not expected to provide protection against developing COVID-19 if exposed to those variants,” the FDA said in a press release explaining why the drug is being pulled.
“Today’s action to limit the use of Evusheld prevents exposing patients to possible side effects of Evusheld such as allergic reactions, which can be potentially serious, at a time when fewer than 10 percent of circulating variants in the U.S. causing infection are susceptible to the product,” the press release stated.
AstraZeneca, the British-Swedish drug giant that also makes a commonly used COVID-19 vaccine, said it was informed that the agency will decide about reinstating authorization of Evusheld if the prevalence of resistant variants in the United States decreases to 90 percent or less on a sustained basis. The drugmaker plans to continue to share relevant data with the FDA and other health authorities regarding Evusheld and SARS-CoV-2 variants.
Monoclonal antibodies act by binding to the spike protein on the surface of the SARS-CoV-2 virus, but the virus has been evolving, causing changes in this protein and affecting how the antibodies work against them.
“AstraZeneca will continue to work with the FDA and other health authorities to collect, assess and share relevant data regarding Evusheld and SARS-CoV-2 variants,” the first said in a statement. “Evusheld currently remains authorized in other countries where it is approved for COVID-19 pre-exposure prophylaxis and treatment, including the EU and Japan.”
In November, the U.S. health regulator also pulled emergency use authorization for Eli Lilly and Co’s COVID-19 drug bebtelovimab, citing similar concerns.