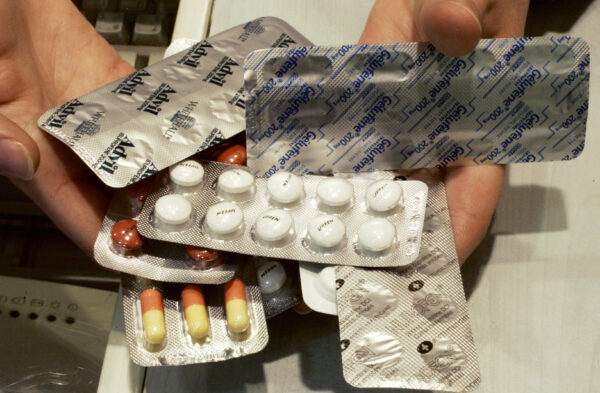
![]() While ibuprofen and acetaminophen remain among the most commonly used drugs in the United States, new research published this week suggests that these over-the-counter medications may be fueling antibiotic resistance.
While ibuprofen and acetaminophen remain among the most commonly used drugs in the United States, new research published this week suggests that these over-the-counter medications may be fueling antibiotic resistance.
The researchers studied what happens when bacteria are exposed to those non-antibiotic drugs in combination with ciprofloxacin, a powerful antibiotic used to treat a range of bacterial infections.
Of those nine drugs, “findings showed that ibuprofen and acetaminophen significantly increased mutation frequency and conferred high-level ciprofloxacin resistance,” researchers said.
They noted that the resistance to antibiotics was more acute in individuals who combined ibuprofen, the active ingredient in Advil, and acetaminophen, commonly sold as Tylenol in the United States and known as paracetamol in other countries.
“Antibiotics have long been vital in treating infectious diseases, but their widespread overuse and misuse have driven a global rise in antibiotic-resistant bacteria,” Rietie Venter, an associate professor and lead researcher in the study, said in the statement.
“This is especially prevalent in residential aged care facilities, where older people are more likely to be prescribed multiple medications—not just antibiotics, but also drugs for pain, sleep, or blood pressure—making it an ideal breeding ground for gut bacteria to become resistant to antibiotics.”
Venter added that bacteria “were not only resistant to the antibiotic ciprofloxacin, but increased resistance was also observed to multiple other antibiotics from different classes.”
The study, he said, shows that officials need to consider the risks of using multiple medications simultaneously, particularly among older adults receiving long-term treatments.
The researchers also called for more studies into antibiotic resistance and non-antibiotic medications.
The U.N. health body said that the overuse of antibiotics in both animals and people has driven the development of bacterial and fungal strains that are resistant to the drugs.
“Antimicrobial-resistant infections that require the use of second- and third-line treatments can harm patients by causing serious side effects, such as organ failure and prolong care and recovery, sometimes for months,” the CDC says on its website.
CDC officials also say that to curb the proliferation of antimicrobial-resistant strains, people are advised to take antibiotics only when they are needed.