What Are the Types of Lung Cancer?
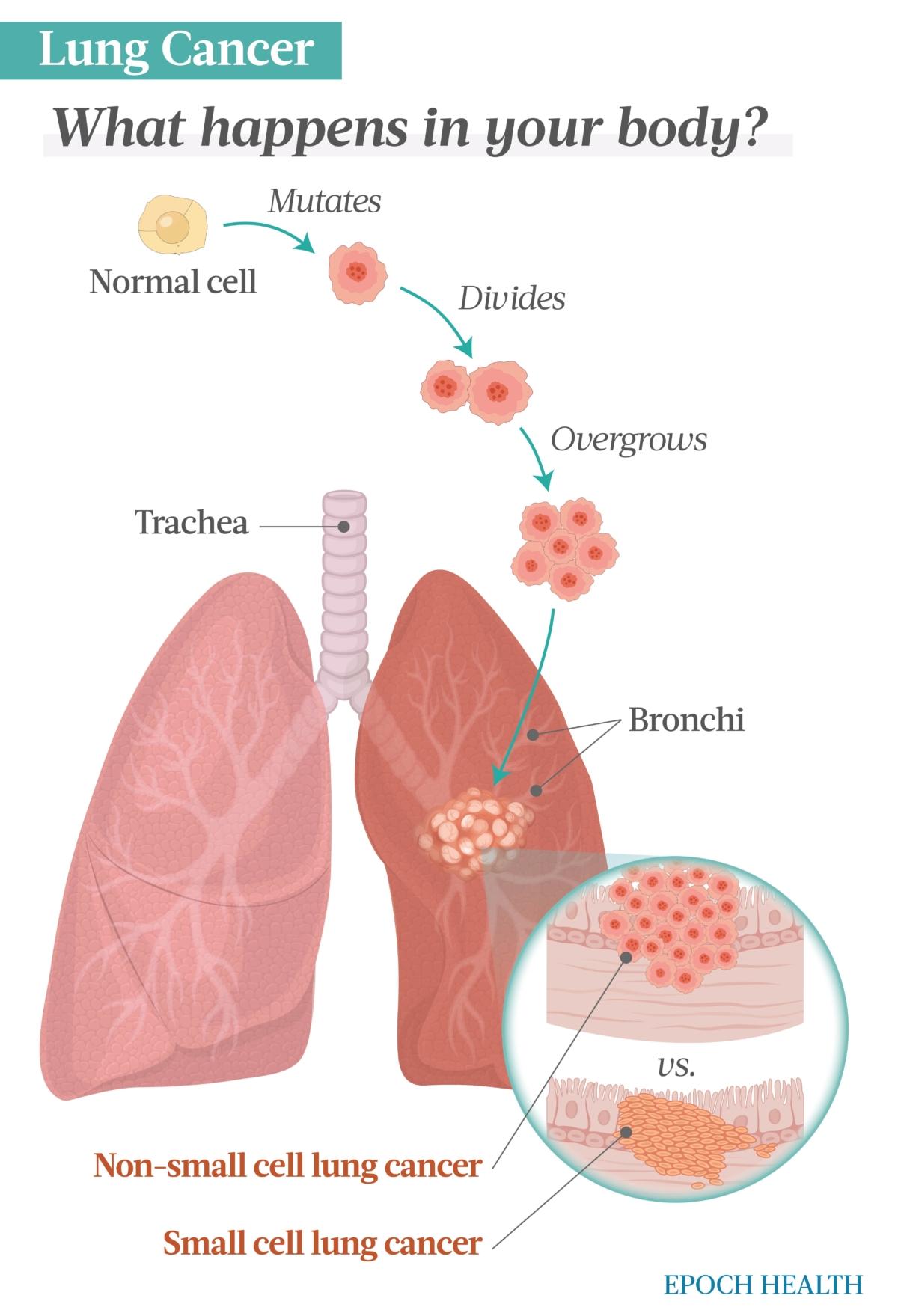
There are two main kinds of lung cancer: non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC), so named for the size of their cells.
1. Non-Small Cell Lung Cancer (NSCLC)
Accounting for 80 percent to 85 percent of all lung cancer cases, NSCLC is any type of epithelial lung cancer not considered small cell lung cancer (SCLC). NSCLC can be further categorized into several subtypes, including unclassified carcinomas:
- Adenocarcinoma: Typically, this subtype originates within glandular cells situated on the lung’s outer periphery. It accounts for 40 percent of all lung cancers.
- Squamous cell carcinoma: Also known as epidermoid carcinoma, this subtype may initiate in flat, delicate cells known as squamous cells, which form the lining of bronchi, the air passages that extend from the trachea (windpipe) into the lungs. This subtype has a more robust association with smoking than other NSCLC types, accounting for 25 percent of all lung cancers.
- Large cell carcinoma: This subtype is an undifferentiated malignant tumor that does not exhibit the distinctive cytological traits of squamous cell carcinoma, adenocarcinoma, or small cell carcinoma. Typically exhibiting a faster growth rate than other non-small cell cancers, it can appear in any part of the lungs and accounts for 10 percent of all lung cancers.
2. Small Cell Lung Cancer (SCLC)
Originating primarily in the bronchial lining cells at the lungs’ center, SCLC is a highly aggressive cancer that can metastasize to distant body regions. Predominantly observed among heavy smokers, it constitutes approximately 10 to 15 percent of all lung cancers. It has two main subtypes:
- Small cell carcinoma, also known as oat cell cancer.
- Combined small cell carcinoma, a mixed tumor involving squamous or glandular cells.
In addition to the main categories, there are other rarer types of lung cancer, including:
- Lung carcinoid tumors, which start in the neuroendocrine cells in the lungs and typically grow slowly.
- Other lung tumors, which are tumors that include adenoid cystic carcinomas (from salivary gland-like cells in the trachea or bronchi), lymphomas, sarcomas, and benign lung tumors (e.g., hamartomas).
What Are the Symptoms and Early Signs of Lung Cancer?
In its initial stages, lung cancer may not exhibit any noticeable signs or symptoms. As the tumor progresses, signs and symptoms tend to emerge.
- Worsening or persistent cough (lasting over three weeks).
- Breathlessness.
- Persistent chest pain that intensifies with deep breaths or coughing.
- Persistent shoulder pain.
- Wheezing.
- Unexplained weight loss.
- Constant fatigue.
- Trouble swallowing.
- Enlarged lymph nodes in the neck, above the collarbone.
- Presence of blood in coughed-up mucus.
- Headaches.
- Night sweats.
- Recurrent chest infections.
- Alterations in voice, such as hoarseness.
- Finger and/or toe clubbing.
- Superior vena cava syndrome (swelling of the face and neck from the tumor pressing on a large vein in the chest).
- Spinal cord compression: Bladder or bowel control disturbances and/or limb weakness may appear from the tumor pressing on the spinal cord.
NSCLC-Specific Symptoms
Horner syndrome can occur when NSCLC forms a tumor in the uppermost part of one lung (Pancoast tumor). The tumor can then damage the sympathetic nerve and cause the eye on that side to have a drooping upper eyelid and a constricted pupil. That side of the face may also be unable to sweat and may have a pink flush compared to the other side.
SCLC-Specific Symptoms
SCLC is more likely than NSCLC to cause paraneoplastic syndromes, a collection of symptoms arising simultaneously with the cancer. These syndromes and symptoms include:
- Syndrome of inappropriate anti-diuretic hormone (SIADH): If the cancer cells make anti-diuretic hormone (ADH), the kidneys retain water, resulting in reduced salt levels within the bloodstream. Major symptoms include muscle weakness or cramping, loss of appetite, restlessness, confusion, fatigue, nausea, and vomiting. It can cause seizures and comas in severe cases.
- Cushing syndrome: When cancer cells produce adrenocorticotropic hormone (ACTH), the body produces excessive amounts of cortisol. Symptoms include elevated blood pressure and blood sugar, a rounded facial appearance combined with thin, weak limbs. It also leads to weight gain in the abdomen, resulting in the development of purple marks there.
- Lambert-Eaton syndrome: This is thought to result from the tumor-inducing antibodies against the communication between muscle and nerve. Symptoms include muscular weakness, diminished mobility, and challenges in activities such as getting up from a sitting position, climbing stairs, or lifting objects.
- Hypercalcemia: This condition occurs when there are elevated calcium levels in the blood, resulting in frequent urination, increased thirst, constipation, fatigue, dizziness, and cognitive confusion.
- Blood clots.
What Causes Lung Cancer?
As with all cancers, lung cancer is caused by the rapid division of abnormal cells that may eventually become tumors or spread via the bloodstream or lymph nodes. Various environmental and genetic factors can damage cells, provoking this abnormal cell division.
Smoking
Cigarette smoking is the leading cause of lung cancer, responsible for over 70 percent of cases and approximately 80 percent of lung cancer deaths. Smokers face a lung cancer mortality risk 25 times higher than those who have never smoked.
Secondhand Smoking
The inhalation of secondhand smoke is called passive smoking or involuntary exposure. Even short periods of exposure can initiate cellular damage that contributes to cancer onset.
Radon Gas
Radon exposure is the second primary cause of lung cancer and the leading environmental cause of any cancer in the United States.
Radon is a colorless, tasteless, odorless, naturally occurring but radioactive gas originating from the natural breakdown of uranium, thorium, and radium in rocks and soil. It enters buildings through cracks or openings and may accumulate indoors. Radon levels are typically highest in basements and on first floors due to their proximity to the ground.
Asbestos and Other Substances
Exposure to the following chemicals increases the risk for lung cancer:
- Asbestos: Inhalation of these naturally occurring fibers can lead to their entrapment within the lungs. Asbestos has been used in building materials (e.g., roofing shingles and asbestos cement products), friction products (e.g., brake and transmission parts), and heat-resistant fabrics.
- Cadmium: Cadmium, a natural element present in small quantities, is mainly obtained in the United States as a byproduct of producing metals like zinc, lead, and copper. As it is resistant to corrosion, cadmium has been utilized in making batteries, pigments, metal coatings, and plastics. Cadmium is also present in tobacco smoke.
- Arsenic: Arsenic, a naturally existing semi-metal, is extensively dispersed throughout the Earth’s crust. Currently, in the United States, copper chromated arsenic (CCA) is used in industrial applications, while organic arsenic compounds find use mainly as pesticides, primarily on cotton plants. Arsenic can enter drinking water from natural sources, and is present in tobacco smoke.
- Chromium: The natural chemical element chromium serves various purposes, including its use in steel production, chrome plating, dye and pigment creation, leather tanning, and wood preservation.
- Silica: Quartz, found in sand, gravel, clay, granite, and various rocks, represents the predominant crystalline silica form, which is hazardous to the lungs. Currently, millions of U.S. workers are exposed to respirable crystalline silica in a variety of industries.
- Diesel exhaust: Several studies involving workers exposed to diesel exhaust have revealed slight yet noteworthy rises in lung cancer risk.
- Polluted air: In a study examining almost half a million people from England, South Korea, and Taiwan, about half of the nonsmokers were found to have a mutation in a gene called EGFR. Researchers found that inhaling tiny air particles called PM 2.5 can increase the chances of getting NSCLC, especially in those with EGFR gene mutations.
Genetics
If your parents, siblings, or children have had lung cancer, your risk of developing it could increase. Studies indicate that certain families have a notable history of lung cancer, possibly due to a gene mutation. For instance, individuals who inherit specific DNA alterations on a specific chromosome (e.g., chromosome 6) are more likely to develop lung cancer, regardless of smoking status.
What Are the Stages of Lung Cancer?
Staging categorizes cancer based on its spread within the body, considering tumor size and location. NSCLC and SCLC have their own separate staging systems.
NSCLC
The TNM system is the most widely used staging system for NSCLC, consisting of five stages. In this system:
- T indicates the size and extent of the primary tumor.
- N indicates the presence of cancer in nearby lymph nodes.
- M indicates if the cancer has metastasized to other body parts.
Combining the T, N, and M situations yields an overall stage for NSCLC:
- Stage 0: This is the earliest stage where cancer cells are found only in the top layer of cells lining the air passages and have not invaded deeper into the lung tissue.
- Stage 1: The lung cancer remains within the lung.
- Stage 2: The lung cancer remains within the lung, but the tumor is larger and more invasive than stage 1.
- Stage 3: At this stage, the cancer has typically spread to nearby lymph nodes and may involve more extensive invasion into the surrounding tissues.
- Stage 4: This is the most advanced stage, indicating that cancer has metastasized to distant organs or tissues.
SCLC
There are two stages of SCLC:
- Limited stage: The cancer exists in one lung and/or in its nearby lymph nodes on the same side of the chest.
- Extensive stage: The cancer has spread extensively within the lung containing the tumor, to the opposite lung, to lymph nodes on the opposite side of the chest, or distant parts of the body. This may also involve cancer spreading to the fluid surrounding the lung.
Who Is More Likely to Develop Lung Cancer?
The risk factors for lung cancer include:
- Smoking.
- Radon exposure.
- Exposure to asbestos and other substances: People who work in asbestos mines, the auto industry, shipyards, cement plants, plumbing and heating trades, construction, and painters, carpenters, and electricians are susceptible to exposure.
- Polluted air exposure.
- High-red meat and/or saturated-fat diet: One review of studies found consuming red meat may increase the likelihood of developing lung cancer, whereas processed and white meats, organ meats, and fish do not appear to contribute to the risk. High consumption of total and saturated fats has been linked to a higher risk of lung cancer, particularly among smokers.
- Older age: It is rare for those under 40 to have this type of cancer.
- Ethnicity: Black men have a roughly 12 percent higher likelihood of developing lung cancer than white men, whereas the rate is approximately 16 percent lower for black women than for white women. While the overall risk of lung cancer is lower among Asian Americans, Native Hawaiians, and Pacific Islanders, it is this group’s primary cause of cancer-related mortality. Among these, Native Hawaiians exhibit the highest lung cancer death rates.
- Personal or family history: Individuals who previously had lung cancer face an elevated chance of recurrence. Around 8 percent of lung cancers stem from inheritance or a genetic predisposition, such as chromosome 6.
- Radiation exposure: Cancer survivors who underwent chest radiation therapy face an elevated risk of lung cancer, particularly if they smoke. Individuals exposed to ionizing radiation from atomic bomb detonations or nuclear accidents are more likely to have an increased risk.
- Certain diseases: Ongoing lung disorders, such as chronic obstructive pulmonary disease (COPD), increase the likelihood of lung cancer. Lung cancer risk also increases for people with certain autoimmune disorders, including lupus, rheumatoid arthritis, Crohn’s disease, Graves’ disease/hyperthyroidism, and sarcoidosis.
- Weakened immune system: Although human immunodeficiency virus (HIV) doesn’t cause cancer per se, since it leads to a weakened immune system, people with HIV/acquired immune deficiency syndrome (AIDS) are prone to developing certain types of cancer, including lung. People with a suppressed immune system are also at an increased risk.
- Sedentary lifestyle: Smokers who engaged in vigorous activity at least once a week have been found to have a 29 percent lower likelihood of developing lung cancer compared to those who rarely or never participated in such activities.
- Beta-carotene supplements: Beta carotene is a red-orange pigment found in many plants and an antioxidant that protects the body from damaging molecules called free radicals. However, research has demonstrated a compelling link between beta-carotene supplements and an increased lung cancer risk among smokers. Therefore, smokers are recommended to obtain beta carotene only via natural food sources.
How Is Lung Cancer Diagnosed?
Many different tests can detect and diagnose lung cancer.
Screening
The U.S. Preventive Services Task Force (USPSTF) recommends annual lung cancer screening for individuals between 50 and 80 with a smoking history of 20 pack-years, whether current smokers or those who have quit within the past 15 years. One pack-year corresponds to smoking an average of one pack of cigarettes daily for a year.
Diagnostic Testing
The process typically starts with a consultation with your physician, who will inquire about your symptoms, risk factors, and general health and conduct a physical examination. Based on these findings, your doctor might direct you to a specialist or request tests to assess lung cancer or other potential health concerns. These tests may include:
- Chest X-ray: A chest X-ray is often the first test used to search for any abnormal areas in your lungs by looking at the organs and bones inside your chest.
- CT scan: A computed tomography (CT or CAT) scan is often the second test during the lung cancer diagnosis procedure. This specialized form of X-ray imaging captures detailed images of the lungs. It is more effective in revealing lung tumors compared to standard chest X-rays. Additionally, it can provide information about the dimensions, form, and location of lung tumors and identify enlarged lymph nodes that may harbor metastatic cancer.
- PET scan: A positron emission tomography (PET) scan is a type of nuclear medicine imaging examination that employs radioactive sugar to generate vivid 3D color images, revealing the functioning of your cells. This test is helpful when your doctor suspects the cancer has metastasized but is unsure of its location, and it can also be used in lung cancer staging.
- MRI scan: A magnetic resonance imaging (MRI) scan provides detailed cross-sectional images of soft tissues in the body but employs radio waves and strong magnets instead of X-rays. It is particularly valuable in searching for potential lung cancer spread to the brain, heart, or spinal cord.
- Ultrasound: Ultrasound employs high-frequency sound waves to generate images of body components. It detects fluid accumulation around the lungs and assists in guiding biopsies or the removal of chest cavity fluids.
- Sputum cytology: Sputum, the mucus coughed up from the lungs, is examined under a microscope by a pathologist to detect cancer cells. This process may help identify cancers originating in the major lung airways.
- Biopsy: A biopsy is a procedure where a small tissue or tumor sample is extracted from the body for microscopic examination. It is performed to diagnose lung cancer or determine if an anomaly is cancerous. A biopsy is the most effective method to determine whether lung cancer exists and the extent to which it has spread.
What Are the Complications of Lung Cancer?
Lung cancer’s complications include:
- Blood clots: A great risk of developing deep vein thrombosis (DVT) exists due to the effects of the cancer itself on clotting factors and sometimes due to chemotherapy. In some cases, clots can dislodge and travel to the lungs, resulting in a condition known as pulmonary embolism (PE).
- Paraneoplastic syndromes: These are most prevalent among middle-aged to older adults and are frequently associated with lung cancer.
- Chemotherapy-induced nausea and vomiting.
- Fatigue.
- Shortness of breath: Lung tumors can lead to shortness of breath by obstructing airways, thus hampering airflow. Lung cancer might also lead to pleural effusion, causing fluid accumulation around the lungs and hindering their full expansion. Additionally, lung cancer can reduce red blood cells, affecting oxygen transport.
- Hemoptysis (coughing up blood): Hemoptysis is when you cough up sputum with blood. This blood can come from your lungs or the tubes that bring air to your lungs.
- Cachexia: This is commonly seen in advanced lung cancer patients with associated weight loss, including muscle loss. At diagnosis, 60 percent of patients have noticeably lost weight.
- Anemia: Anemia is common among individuals with lung cancer, with its occurrence and intensity influenced by factors such as the stage of the tumor, duration of the illness, and past and ongoing treatments.
- Neutropenia: Chemotherapy-induced neutropenia refers to a decreased level of neutrophils, a type of white blood cell.
- Nephrotoxicity: Nephrotoxicity is a swift decline in kidney function caused by the toxic impact of medications and chemicals.
- Fluid buildup in the chest.
- Hypercalcemia: In some instances, lung cancer can cause hypercalcemia, which is higher calcium levels in the blood.
What Are the Treatments for Lung Cancer?
Treatment plans depend on the type of lung cancer you have. The following are the main types of treatments, though there are others.
1. Surgery
The surgery option is determined primarily by the tumor’s size, location, and extent of spread within the lungs. If a patient has NSCLC in one lung and is in good health otherwise, surgery to remove cancer cells is likely recommended. Since SCLC often affects both lungs, surgery alone is not commonly recommended. Lymph nodes may also be removed during the surgery to determine if they contain cancer.
- Wedge resection or segmentectomy: This surgery removes a small portion of the lung. It’s only suitable for a select group of patients with small, localized cancers, often at an early stage of NSCLC.
- Lobectomy: This involves removing one of the larger sections (lobes) of the lung. It is usually recommended if the cancer is confined to one specific section of one lung.
- Pneumonectomy: In this procedure, the entire lung is removed. It’s chosen when the cancer is located in the middle of the lung or has extensively spread throughout the lung.
- Sleeve resection: This procedure removes part of the bronchus.
2. Radiation
Radiation therapy employs strong energy beams to help eliminate cancer cells. Sometimes, a combination of chemotherapy and radiation is the primary approach. Radiation therapy can alleviate symptoms like pain for advanced lung cancers or those that have spread.
- External beam radiation therapy (EBRT): EBRT directs radiation from outside the body onto the cancer. This method is painless, with each session taking just a few minutes. Lung radiation treatments are usually administered five days a week over five to seven weeks.
- Internal radiation therapy (brachytherapy): Also known as endobronchial brachytherapy or endobronchial radiation therapy, this is a form of internal radiation therapy. It involves placing radioactive material inside the bronchus during a bronchoscopy. Brachytherapy is utilized for lung tumors in the bronchi and minimizes radiation exposure to nearby organs.
Prophylactic cranial irradiation (PCI), which involves applying external beam radiation to the entire brain, is recommended for individuals with either limited or extensive stage SCLC who have positively responded to chemotherapy and radiation therapy. However, it is not considered for those with SCLC who have not responded to chemotherapy. NSCLC patients do not benefit from this treatment.
3. Chemotherapy
Chemotherapy uses anti-cancer drugs to halt the growth of cancer cells, either by eliminating them or impeding their division. Most people with lung cancer receive chemotherapy depending on their stage or to help eliminate residual cancer cells if surgery is first performed.
After completing the cycles, your doctor will assess the progress. If the cancer has improved, further treatment might not be necessary. If the cancer hasn’t shown improvement, your doctor may recommend a different chemotherapy or maintenance chemotherapy to control the cancer.
Lung cancer chemotherapy involves a combination of medicines delivered through an intravenous drip or a chest tube. Drugs are sometimes given as oral capsules or tablets.
4. Targeted Therapy
Targeted therapy, also called biological therapy, uses medications created to impede the progression of advanced NSCLC. These treatments suit individuals with specific proteins in their cancer cells.
5. Radiofrequency Ablation
Radiofrequency ablation (RFA) may be considered for people with small tumors near a lung’s edge. It uses powerful radio waves to heat the tumor. A thin, needle-like device is inserted through the skin and carefully positioned within the tumor, aided by CT scans. Once properly placed, an electric current flows through the probe, generating heat that eradicates cancer cells within the tumor.
6. Endobronchial Therapy
Endobronchial therapy removes blockages caused by lung cancer within the airway tubes (bronchi or bronchioles). When surgical removal of the cancer isn’t feasible due to health concerns or tumor location, endobronchial therapies can mitigate symptoms by reducing airway blockage.
7. Immunotherapy
Immunotherapy is a biological therapy that uses the patient’s own immune system to fight cancer. Immunotherapy drugs boost, direct, or restore the body’s natural defenses against cancer.
Immune checkpoint inhibitor therapy is an immunotherapy used to treat some patients with advanced NSCLC. One example is the PD-1 and PD-L1 inhibitor therapy.
PD-1 is a protein found on the surface of T cells that helps keep the body’s immune responses in check. PD-L1 is a protein found in some types of cancer cells. When PD-1 attaches to PD-L1, it stops the T cells from killing the cancer cells. PD-1 and PD-L1 inhibitors keep PD-1 and PD-L1 proteins from attaching to each other, thus allowing the T cells to kill cancer cells.
8. Palliative Care
Palliative care, or supportive care, helps manage lung cancer symptoms and treatment side effects. Meeting with a palliative care team early on can ensure comfort during and after treatment.
How Does Mindset Affect Lung Cancer?
Although certain studies indicate that maintaining a positive attitude might not directly influence lung cancer survival rates or disease progression, other research suggests that optimism and a positive mindset can contribute to an improved quality of life for individuals facing cancer.
What Are the Natural Approaches to Lung Cancer?
Natural remedies for lung cancer include some alternative therapies, which can help promote cancer cell death and improve symptoms and treatment side effects, but they are currently intended to complement conventional treatments rather than replace them. Before using any of the following natural remedies, please consult your doctor.
1. Whole-Body Hyperthermia
Also known as thermal therapy, thermal ablation, or thermotherapy for cancer treatment, hyperthermia is a treatment method where body tissue is heated to temperatures as high as 113 F (45 C), aimed at selectively damaging and eliminating cancer cells while sparing healthy tissues.
Hyperthermia can be used to treat many types of cancer, including lung. Hyperthermia can potentially disrupt the structures and proteins within cancer cells, reducing the size of lung tumors. Additionally, hyperthermia might enhance the responsiveness of cancer cells to other therapeutic interventions. It is almost always used with chemotherapy, radiation therapy, or other forms of cancer treatment.
The tools used in hyperthermia treatment include microwave-powered probes, radio waves (radiofrequency), lasers, heated blankets, and a heated chamber.
- Local hyperthermia: Heat is applied to a small area of the body.
- Regional hyperthermia: Heat is applied to an organ, limb, or large area of the body.
- Whole-body hyperthermia: A patient is treated in a thermal chamber or covered with heated blankets, elevating the body temperature to 107 or 108 F for brief durations.
One study found that the combined approach of whole-body hyperthermia along with cytostatic treatment (cyclophosphamide and melatonin) led to the most significant suppression of spontaneous Walker 256 carcinosarcoma tumor growth. This treatment also halted mitotic activity in tumor cells and promoted necrotic and apoptotic cell death. Hyperthermia treatment is currently viewed as a “promising anti-cancer strategy.”
2. Traditional Herbal Medicine
According to a paper in Integrative Cancer Therapies, traditional herbal medicine has long been vital in complementary and alternative medicine, offering multiple targets, minimal side effects, and significant therapeutic advantages.
Jinfukang decoction (JFK), an herbal formula for NSCLC therapy, comprises 12 herbs used in traditional Chinese medicine (TCM). Laboratory studies indicate that JFK prescriptions act as tumor inhibitors in human lung cancer cells by blocking their growth through DNA inhibition. Furthermore, clinical findings reveal that combining the decoction with cisplatin chemotherapy extends survival among stages 2 and 3 NSCLC patients, enhances immune metrics, and mitigates cisplatin-induced side effects.
The paper indicates that certain herbal decoctions can induce cancer cell death, make cells more susceptible to other cancer treatments, reduce tumor recurrence rates, regulate human immune functions, or prolong disease-free survival in patients.
- Astragalus: Astragalus membranaceus polysaccharides (APS), one component of the JFK prescription, have been found to decrease the proliferation and migration of NSCLC cells.
- Berberine: Berberine comes from plants like Chinese medicinal herbs barberry and goldenseal. One study showed that a particular form of berberine called phytantriol-based berberine has about 20 times the strength in stopping lung cancer growth and spread as regular berberine. In lab tests, it also helped control genes related to lung cancer, reducing the activity of proteins that enhance cancer cell growth. It also has fewer side effects than regular berberine.
- White mulberry (Morus alba): Albanol B (ABN-B), isolated from mulberries, has been found to be able to inhibit the proliferation of four human lung cancer cell lines and induce cell death. Treatment with Kuwanon M (KWM), another characteristic constituent isolated from the root bark of Morus alba, can induce the suppression of lung cancer cell proliferation and migration in lab studies.
- Snake-needle grass (Oldenlandia diffusa): In one animal study, this extract effectively suppressed lung cancer cells and triggered a notable increase in their death. Additionally, it significantly inhibited lung metastases without any noticeable adverse effects.
- Curcumin: Curcumin, derived from turmeric, is a key compound with various therapeutic properties, like antioxidants and anti-inflammatory effects. It can be an effective adjunct in treating solid organ tumors due to its ability to regulate oncogenes and its lack of harmful effects. However, most evidence comes from laboratory studies, so more research involving patients is needed to confirm its effectiveness.
- Thai herbal extracts: One study found several extracts of Thai medicinal herbs Bridelia ovata, Croton oblongifolius (dyer’s croton), and Erythrophleum succirubrum that exhibited toxic effects on one lung cancer cell line. The ethanolic extract of E. succirubrum was the most effective and had a significant potential to be used for future lung cancer treatment.
3. Aromatherapy
Aromatherapy uses plant essential oils as a complementary health practice, often inhaled or applied in diluted form on the skin. The essential oils from certain plants have been shown to affect lung cancer cells in laboratory tests and living organisms. One study found that vapor from the essential oils of Litsea cubeba seeds could kill lung cancer cells by inducing their apoptosis and causing cell cycle arrest.
4. Therapies to Potentially Reduce the Use of Chemo Drugs
Several therapies can enhance the efficiency of cancer drug administration, thus making the treatment healthier for patients. These include:
- Insulin potentiation therapy (IPT): Also known as insulin-potentiated targeted low-dose therapy (IPTLD), this offers a complementary approach to treating certain cancers, including lung cancer. Often termed “low-dose chemotherapy,” IPT is a complementary treatment alongside other cancer therapies. As insulin can increase the permeability of cancer cell membranes due to their higher insulin receptor count, this therapy makes it easier for chemotherapy drugs to enter the cancer cells. Then, fewer chemotherapy chemicals are needed for the same therapeutic effects.
- Magnetic aerosol drug targeting (MADT): An emerging technique that shows great promise for lung cancer therapy, MADT involves utilizing a permanent magnet to deliver drugs to specific locations within the lung precisely. MADT can be performed by using either an implanted magnet within the body or a magnet positioned externally. Using a permanent magnet has a noticeable impact on how efficiently treatment particles are trapped.
5. Acupuncture and Acupoint Stimulation
Research has demonstrated that stimulating specific acupoints has a powerful impact on the immune system of lung cancer patients. Researchers observed a notable rise in immune cell-regulating cytokine interleukin-2 levels, as well as an increase in immune cells, including T-cell subtypes and natural killer cells. Moreover, acupoint stimulation notably reduced the bone marrow suppression often caused by conventional therapy in lung cancer patients, including lower hemoglobin, platelet, and white blood cell counts.
How Can I Prevent Lung Cancer?
Based on the risk factors for lung cancer, there are several ways for you to prevent it:
- Avoid or quit smoking or being around secondhand smoke: Within 12 years of quitting, your lung cancer risk will decrease by over half that of a smoker.
- Test your home’s radon levels: You can get the radon level of your home tested by contacting your state radon office.
- Avoid or minimize exposure to carcinogens: Before taking a new job, do your due diligence to determine if there will be exposure to lung cancer-causing toxic substances such as asbestos and silica.
- Eat a lower-fat, high-fiber diet: Choose a diet with lots of fruits, vegetables, and healthy meats. Limit red meat and saturated fats; consume poultry, fish, and vegetables instead. Regular consumption of cruciferous vegetables, such as cabbage, broccoli, and Brussels sprouts, has been shown to protect against lung cancer.
- Get enough omega-3s: The three primary omega-3 fatty acids include alpha-linolenic acid (ALA) found in plant oils, eicosapentaenoic acid (EPA) found in fish and other seafood, and docosahexaenoic acid (DHA) found in seafood. Research suggests that omega-3 fatty acids might hinder the growth of cancer cells and potentially regulate key pathways that influence the advancement or complications of lung cancer.
- Boost your vitamins and antioxidants: Oxidative stress is a key factor in the harmful effects caused by cancer radiation therapy and chemotherapy. Antioxidants such as vitamins A, C, and E, as well as selenium and zinc, can potentially enhance the body’s defense against oxidative stress. On the other hand, laboratory research indicates that very high doses of vitamin C make it act as a pro-oxidant, reducing the energy levels in cancer cells, damaging their DNA, and thus triggering a chain of reactions that eventually leads to their death.
- Exercise at least twice per week: Adults should aim for 150 minutes of moderate-intensity aerobic activity per week, coupled with strength training twice a week.
- Get lung cancer screenings if at high risk: If you are at a high risk of developing lung cancer, talk with your doctor, who will order the appropriate screening tests for you.
Medically reviewed by Beverly Timerding, MD.










